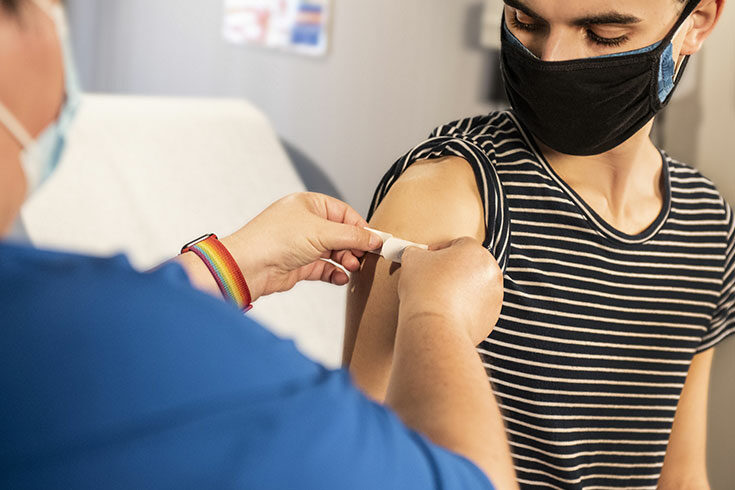
The vaccination clinic is positioned alongside the meals take away service at the front of our property. Every day there are people we have not seen before, there are also regulars and the pattern of use is varied. There are those who come once or twice a month, right up to people who attend almost daily.
The clinic ran twice a week for three hours per session from a large white marquee in the middle of our front courtyard.
We have privileged a consistent, single worker to act as a vaccine ambassador. This has enabled consistent messaging and allowed the worker to become a familiar and trusted source of information.
This worker does a range of things including meeting and greeting arrivals, inviting people to have a vaccination, answering questions, and providing written information. A major part of the role has been listening to people’s fears and concerns. Having a single worker present for each session has been a key part of this project’s success.
I’d like to also acknowledge the work of STAR Health and particularly the team who have been coming to our service, who have demonstrated great flexibility and patience and an openness to working in a spontaneous way.
We know that in our four residential services, vaccination uptake has been high (above 80%). This is primarily because workers have increased opportunities and time to engage with residents. At a drop-in service like ours, with an ever-renewing community of transient and marginalised people, the fully vaccinated rate remains low and (at the time of writing) is still under 50%.
While many people in the homeless community are mindful of their health, we know that homelessness itself has a diversity of presentations. There are groups of people within this community who do not often engage with services. Experiences of trauma are probably at the heart of this.